Focused shockwave therapy has gradually evolved from a traditional physical rehabilitation method into a treatment technology with “regenerative medicine attributes” in recent years. Its core lies not in simple mechanical stimulation, but in the formation of specific physical and biological response couplings within tissues through highly controllable energy transfer, thereby triggering repair, reconstruction, and even functional recovery processes.
Unlike conventional physiotherapy equipment, the key advantage of focused shockwave therapy lies in its “spatial selectivity.” Energy is not dissipated on the surface, but rather achieves maximum deposition in a predetermined focal area within the body. This ability to “deeply target specific areas” gives it clinical value that is difficult for traditional techniques to replace in treating chronic injuries, blood flow disorders, and soft tissue degeneration.
Physical Fundamentals of Shockwave Therapy
From a physical perspective, a shockwave is a transient pressure wave with significantly nonlinear characteristics. Its difference from ordinary sound waves lies not in “greater intensity,” but in its completely different propagation mode and energy release mechanism. Shock waves exhibit extremely rapid pressure rise during propagation, typically reaching peak pressure within nanoseconds. This rapid energy loading creates significant stress concentration in tissues, triggering a series of mechanical responses.
Simultaneously, shock wave propagation is accompanied by a negative pressure phase, which generates cavitation in the liquid environment. The formation and collapse of bubbles not only alter the local hydrodynamic environment but also further enhance mechanical stimulation at the cellular level. This combination of “positive pressure shock + cavitation effect” enables shock waves to act simultaneously on cellular structures and the tissue microenvironment.
Therefore, from a therapeutic mechanism perspective, shock waves are not a single mode of action but rather a complex yet highly controllable energy transfer system formed through the superposition of multiple physical processes.
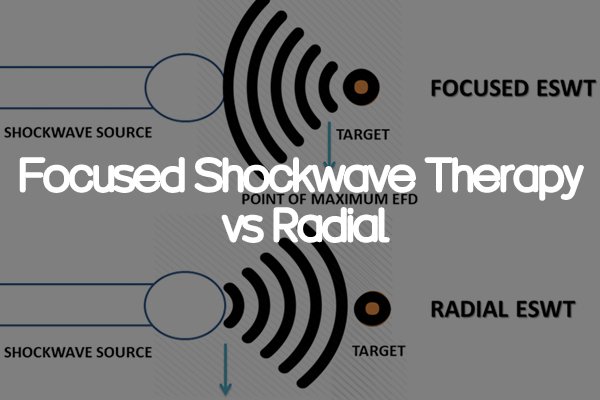
Focused vs Radial Shockwave: A Structural Difference Rather Than a Gradient
In clinical and marketing contexts, focused and radial shock waves are often simply understood as a difference between “deep” and “shallow” layers, but this explanation ignores a more fundamental physical difference. The core difference lies not in the magnitude of energy but in the spatial distribution of that energy. Focused shockwaves, through acoustic lenses or reflective structures, cause energy to gradually converge along its propagation path, reaching a peak at a specific focal point. This means that upon entering the body, the energy does not rapidly attenuate at the surface but rather “penetrates” to the target depth before being released in a concentrated manner. This mechanism allows it to effectively act on deep structures without significantly affecting superficial tissues.
In contrast, divergent shockwaves reach their maximum energy instantaneously upon generation and then diffuse radially outward, with their energy density decreasing exponentially with depth. This characteristic makes them more suitable for mechanical stimulation of superficial tissues and less effective at generating sufficient therapeutic intensity in deeper regions.
From a clinical perspective, this structural difference further manifests as functional differentiation: focused shockwaves tend to participate in tissue repair and regeneration processes, while divergent shockwaves are more often used for short-term pain modulation. This difference is not a matter of “superiority or inferiority,” but rather a distribution of indications directly determined by the physical mechanisms.
Energy Generation Mechanisms and Their Clinical Implications
The generation of focused shockwaves relies on the efficient conversion of electrical energy into mechanical energy, a process that can be achieved through different technological pathways. Electromagnetic systems generate sound waves by using an electric current to create a magnetic field, which drives a metal diaphragm to move rapidly. The sound waves are then focused using a lens structure. This technology offers stable output and high controllability, making it widely used in modern equipment.
Piezoelectric systems rely on a large number of piezoelectric crystals that deform synchronously under the influence of an electrical signal to directly generate and focus sound waves. This method offers significant advantages in spatial focusing accuracy, but due to its complex structure, its application is primarily limited to high-precision medical scenarios.
Electro-hydraulic systems, as one of the earliest applied technologies, generate shock waves by producing electrical sparks in a liquid. They have high peak energy, but exhibit some fluctuations in repeatability and stability.
It is important to emphasize that “focused shock waves” are not synonymous with any single technology, but rather represent a result achieved through the combined design of these technologies—namely, the formation of a controllable focal energy distribution within the body. Therefore, in practical applications, the choice of technology primarily affects the stability and parameter consistency of the equipment, rather than whether focusing can be achieved.
Biological Mechanisms: From Mechanical Stimulus to Tissue Regeneration
The clinical efficacy of shockwave therapy essentially stems from its “mechanical activation” of biological systems. When shockwaves act on tissues, the cell membrane and its associated mechanosensory structures are the first to be affected. These structures convert external mechanical forces into intracellular biological signals—a process known as mechanotransduction.
During this process, multiple signaling pathways are activated, including key regulatory pathways such as MAPK, ERK, and PI3K/Akt. These signals further regulate gene expression, inducing cells to proliferate, migrate, or differentiate, thus providing a foundation for tissue repair.
At the vascular system level, shockwaves can significantly promote the expression of angiogenesis-related factors, such as VEGF and eNOS. Upregulation of these factors promotes the formation of new capillaries and improves local blood flow and oxygen supply. This mechanism is particularly crucial in treating vascular-related diseases such as erectile dysfunction because it directly addresses the pathological basis of the disease.
Furthermore, shockwaves also have a profound impact on connective tissue. By stimulating fibroblast activity, it can promote collagen synthesis and remodeling, thereby improving tissue structure and mechanical properties. This structural change is an important source of long-term efficacy.
At the nervous system level, shockwave therapy can achieve sustained analgesia by modulating the release of pain mediators and neural conduction pathways. Unlike traditional analgesia methods, this modulation does not simply inhibit signals, but achieves deeper functional remodeling by altering nerve sensitivity.
Clinical Evidence and Indications
With the continuous accumulation of research, focused shockwave therapy has gained substantial evidence support in multiple medical fields. In musculoskeletal disorders, its efficacy in chronic tendinitis, plantar fasciitis, and rotator cuff injuries has been validated by numerous randomized controlled trials. These studies generally show that, compared to conservative treatment alone, shockwave therapy can significantly improve pain scores and promote functional recovery.
In the urology field, low-intensity focused shockwave therapy has become an important research direction for vascular erectile dysfunction. Extensive clinical data indicate that this therapy can significantly improve patients’ functional scores by improving blood flow to the corpora cavernosa, and its effects are sustained in specific populations. In addition, shockwave therapy is increasingly being incorporated into multidisciplinary treatment plans for chronic pain and soft tissue repair. Its non-invasive nature makes it an important option between drug therapy and surgical intervention.
Standardized Treatment Protocols
Although the mechanism of shockwave therapy is relatively well understood, its clinical efficacy largely depends on parameter settings and treatment strategies. Energy flux density is the most critical control variable; different energy levels correspond to different biological effects: lower energy is typically used to promote tissue regeneration, while higher energy is more suitable for breaking down calcifications or stimulating strong responses.
During treatment, the number and frequency of pulses jointly determine the total energy input and treatment efficiency, while the treatment interval affects the tissue recovery rhythm. Overly frequent treatments may lead to excessive tissue stress responses, while excessively long intervals may weaken the cumulative effect.
In deep tissue treatment, image guidance is gradually becoming a key means to improve the consistency of efficacy. Ultrasound localization ensures that energy is precisely applied to the lesion area, thereby reducing the impact of individual differences.
Clinical Decision-Making and Patient Selection
In clinical practice, the application of shockwave therapy is not suitable for all patients. Its optimal target population is typically patients with chronic disease, especially those who do not respond well to traditional conservative treatments but have not yet met the criteria for surgery. This positioning places it in a crucial “intermediate intervention” position within the treatment pathway.
Simultaneously, the identification of contraindications is equally important. For example, shockwave therapy may pose potential risks in the presence of tumors, coagulation disorders, or acute infections. Therefore, appropriate patient selection not only affects efficacy but also directly relates to treatment safety.
Focused Shockwave Therapy represents a treatment paradigm shift from “physical stimulation” to “biomodulation.” Its value is not limited to short-term symptom relief but lies in achieving long-term improvements in tissue structure and function through multi-level mechanisms.
With advancements in equipment technology and in-depth clinical research, this therapy is gradually moving from empirical application to standardization and precision. In the future, its development will focus more on individualized parameter optimization and the combined application of multiple technologies, thereby further expanding its potential in regenerative medicine.